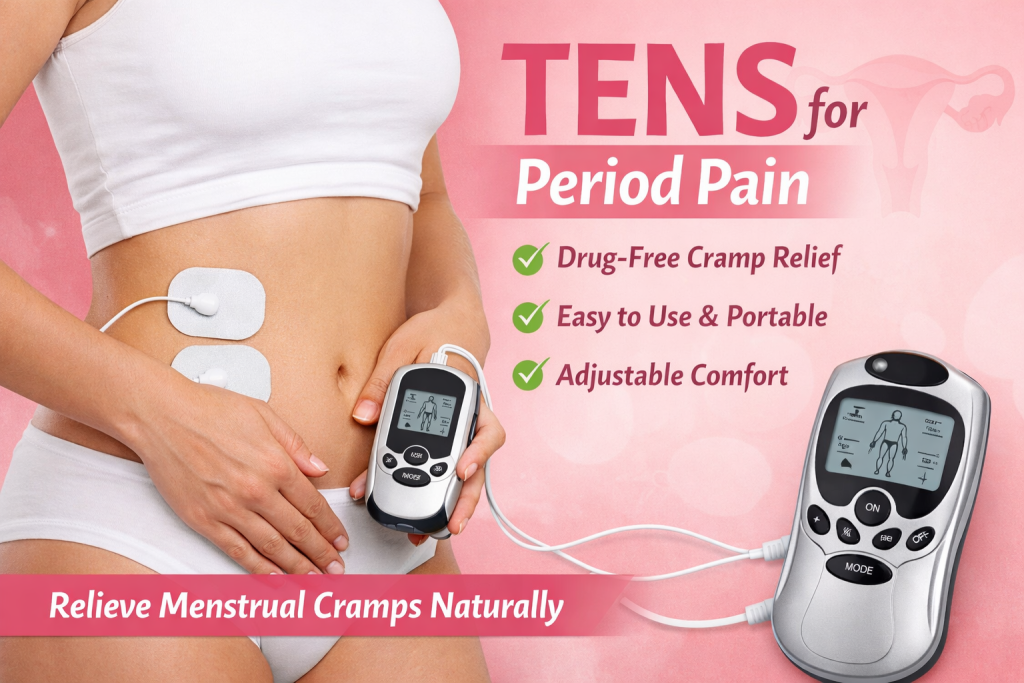
Period (menstrual) pain-primary dysmenorrhoea-can be painful and disruptive. A TENS (transcutaneous electrical nerve stimulation) machine is a non-drug, portable option many people use to reduce cramping and discomfort. Below is a complete, practical guide: what TENS does, what the evidence says, how to use it safely and effectively, and when to seek medical help.
Expert opinion: TENS devices are not only for pain relief but can also be used during normal daily routines for general relaxation and massage. Gentle electrical stimulation helps ease muscle tension, support circulation, and reduce everyday stress and fatigue when used at a comfortable intensity.
What is TENS and how it helps:
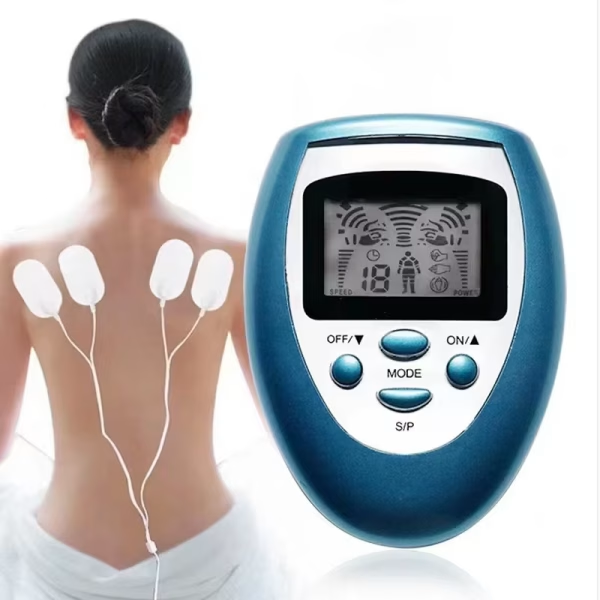
A TENS unit delivers mild electrical pulses through adhesive pads on the skin. These pulses can block or alter pain signals travelling to the brain and may stimulate the release of endorphins (your body’s natural painkillers). Many people report faster, drug-free relief of cramping and muscle tension when they use TENS correctly.
What the evidence says:
Systematic reviews of randomized trials conclude that both high- and low-frequency TENS may reduce menstrual pain compared with placebo or no treatment, though the certainty of the evidence is rated low to moderate and not everyone benefits. In short: TENS can help for many people, but results vary and more high-quality research is still needed.
Benefits you might expect:
- Rapid relief of cramping during a session (some users feel relief immediately).
- A drug-free option useful when you want to avoid or reduce painkillers.
- Portable and simple to use at home, work, or school.
- Can be combined with other approaches (NSAIDs, heat packs, relaxation) for better control.
How to use a TENS unit for period pain – step-by-step
- Read the manual first. Every device differs slightly — check battery/charging, pad types, and control layout.
- Skin prep. Clean and dry the skin where you’ll place pads; avoid oils or lotions.
- Pad placement (common, effective setups):
- Two pads on the lower abdomen (one each side of the midline, just above the pubic bone), or
- One pad on the lower abdomen and one on the lower back (over the sacral/lumbar area) to form a current path across the painful area.
Do not place pads over the genitals or inside body orifices.
- Start low and increase slowly. Turn the unit on at the lowest setting and raise intensity until you feel a comfortable tingling — never set it to a painful level.
- Duration & frequency: Typical sessions are 20–30 minutes, and many users do up to 3–4 sessions per day during peak pain. If relief wanes, try short breaks or change pad placement.
- Finish safely. Turn the device off before removing pads to avoid strong stimulation on removal. Clean and replace pads as manufacturer recommends.
Safety, precautions & who should consult a clinician
- Do not use TENS if you have an implanted electrical device (e.g., pacemaker, defibrillator) unless cleared by the device manufacturer and your clinician.
- Pregnancy: If you are pregnant, check with your healthcare provider first. (TENS is used in labour under some circumstances, but pregnancy requires professional advice.)
- Avoid placing pads over broken/irritated skin, the front of the neck, eyes, chest/heart area, or across the head. Do not use internally unless the device is designed and clinically approved for that use.
- Stop use and seek help if you experience sharp pain, numbness, dizziness, burn or skin reaction, or worsening symptoms.
- If you have underlying conditions (epilepsy, cardiac disease, undiagnosed pelvic pain, recent pelvic surgery, or active infection), get medical advice before using TENS.
Practical tips & troubleshooting
- Replace hydrogel pads or keep them clean — worn pads reduce effectiveness.
- If you feel nothing, check pad contact, battery charge, and that the unit is on the correct mode.
- If TENS stops helping after long-term use, try a short break (a few days) — some users report tolerance builds up.
- Pair TENS with heat, relaxation breathing, or an NSAID (if appropriate) for extra relief — ask your clinician about safe medication combos.
When to see a doctor instead of relying on TENS
- Severe pain that prevents normal activity despite TENS and usual treatments.
- Very heavy bleeding or irregular bleeding, or any sudden changes in your cycle.
- New or unusual pelvic symptoms (fever, severe nausea, fainting).
If period pain is consistently severe, a doctor can check for underlying causes (endometriosis, fibroids, pelvic inflammatory disease) and advise a tailored treatment plan.
Quick FAQ
- Is TENS safe long-term? Generally yes for most users, but follow device instructions and check with a clinician if you have chronic health issues.
- Will TENS replace painkillers? Sometimes – for some people TENS reduces or replaces analgesics; for others it’s an adjunct.
- Can everyone use it? Not everyone: see safety section (pacemaker, pregnancy, certain skin or pelvic conditions).